Key Statistics
Did you know? A gallon of water weighs about 8.3 lb (3.8 kg). For example, consuming this much fluid quickly can strain your cardiovascular system and kidneys. Moreover, emergency departments report rising cases of water intoxication among teens and young adults participating in viral hydration challenges.
How Do Gallon Water Bottles Cause Health Problems?
Gallon jugs (128 oz) normalize rapid, excessive drinking. As a result, attempting a full gallon in a short window can overwhelm water-balance mechanisms and dangerously dilute blood sodium.
The Viral “Gallon Challenge” Risk
Furthermore, social media challenges push people to drink far beyond individual needs, ignoring safe limits and medical nuance.
Understanding Gallon Water Bottle Dangers
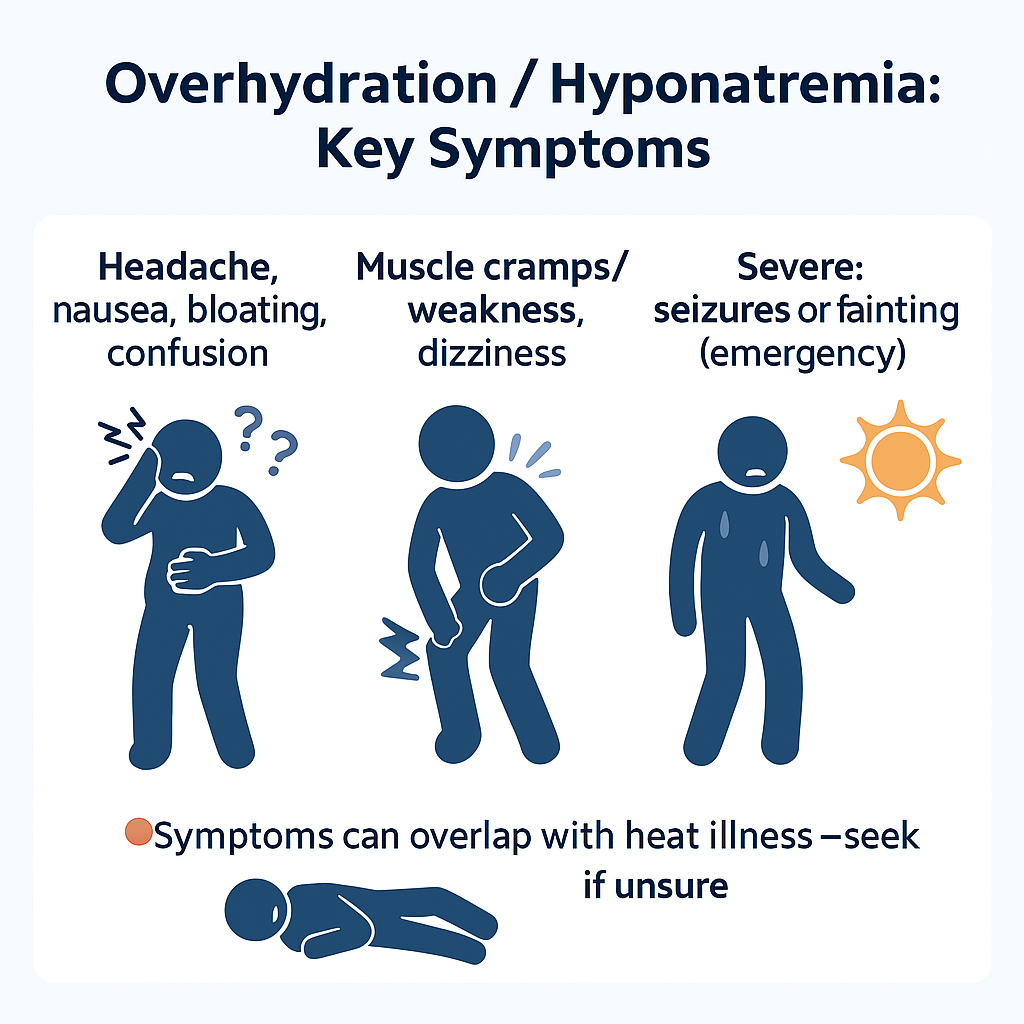
On campuses and in gyms, “who can drink more?” games can quickly cause hyponatremia. Specifically, symptoms include headache, nausea, confusion, and—if severe—seizures. In addition, similar patterns are documented in marathoners, military trainees, and recreational athletes.
The Science Behind Hydration
Hydration is more than total volume—it’s the balance of water and electrolytes across body fluids and tissues. Therefore, practical plans should consider both fluid and sodium.
Note: Some hypotheses (e.g., “exclusion zone” water) are debated; nevertheless, clinical recommendations rely on established physiology and consensus guidelines.
What Overhydration Does: Water Intoxication Explained
- First, it drops blood sodium below normal.
- Next, water moves into cells (including brain), causing swelling.
- As a result, headache, nausea, confusion, and muscle weakness can occur.
- In severe cases, seizures, coma, or death may follow.
- Additionally, it can mimic heat illness, delaying recognition.
A landmark study of Boston Marathon runners linked hyponatremia to weight gain from overdrinking; moreover, additional research suggests overhydration is often riskier than mild dehydration for most athletes.
Dangerous Water Consumption: Red Flags to Watch For
Before you set a daily goal, consider the warning signs below; importantly, several of them indicate that your intake may already be too high.
- More than 1 gallon (128 oz) daily as a routine goal
- More than ~1 liter (34 oz) per hour for several consecutive hours
- Clear urine all day
- Headache, nausea, bloating, or confusion after large intakes
- Peer pressure to “keep up” or “finish the jug”
- Drinking when not thirsty
Exercise guidance: a common range is ~0.4–0.8 L/hour unless a sports medicine professional advises otherwise. In practice, “drink to thirst” prevents both under- and over-hydration more effectively than rigid schedules.
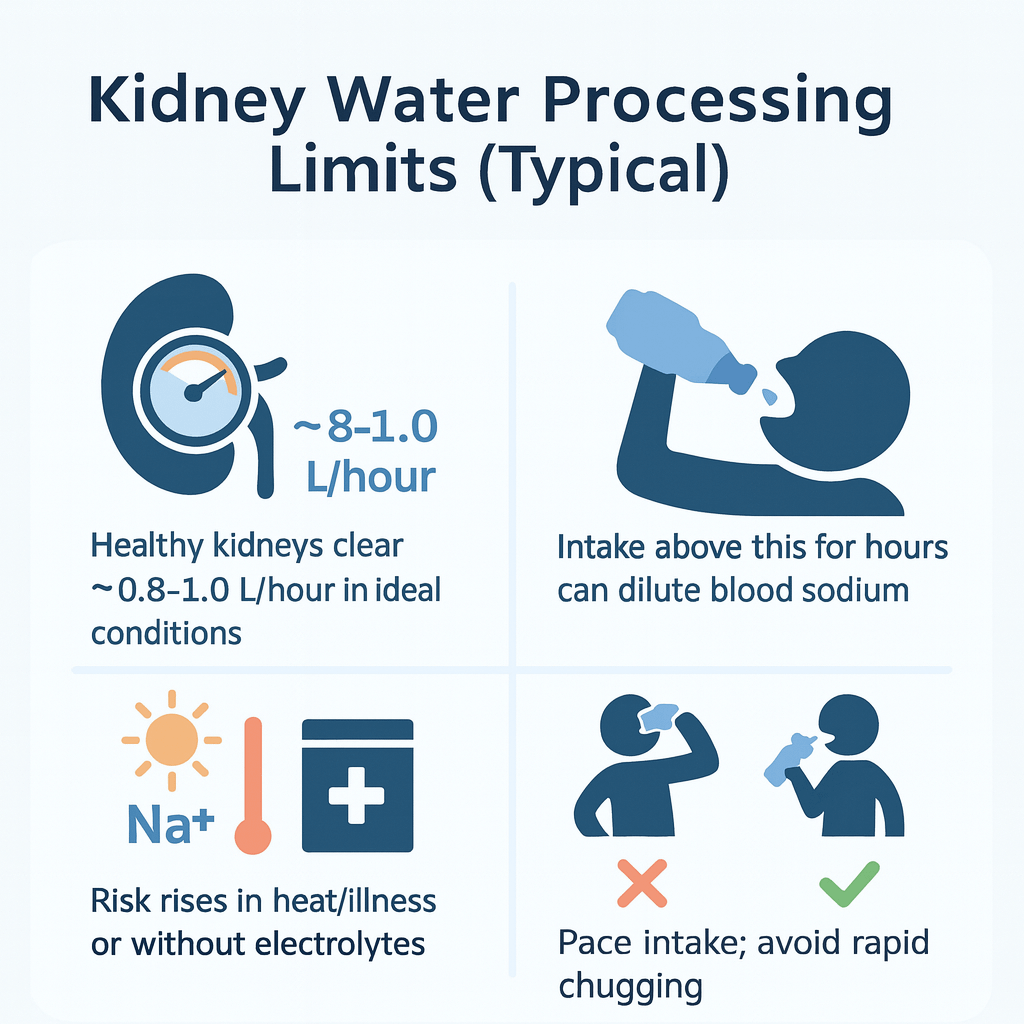
Kidney Water Processing: Understanding Your Body’s Limits
In ideal conditions, healthy kidneys can sometimes excrete roughly 0.8–1.0 liters per hour. However, rapid intake—especially without electrolytes—raises risk.
Clinician Note: What That “0.8–1.0 L/hour” Really Means
Context matters. In healthy adults, kidneys can excrete up to ~0.8–1.0 L/hour of very dilute urine when antidiuretic hormone (ADH/AVP) is low and dietary solute (sodium/protein) is adequate. During exercise, heat, pain, nausea, or stress, ADH rises, which reduces water clearance—therefore, your practical hourly limit is often lower.
- Solute matters: very low sodium/protein intake lowers maximum free-water excretion.
- Real-world guidance: consequently, drink to thirst, avoid rapid chugging, and avoid body-weight gain during long events.
| Time Period | Water Consumed | Risk Level | What Happens |
|---|---|---|---|
| 1 hour | 24–32 oz (0.7–1.0 L) | Safe Zone | Within typical clearance capacity |
| 2 hours | 48–64 oz (1.4–1.9 L) | Yellow Flag | Approaching clearance limit |
| 3 hours | 72–96 oz (2.1–2.8 L) | Red Flag | Exceeding clearance—dilution risk rises |
| 4 hours | 128 oz (3.8 L / 1 gallon) | Danger Zone | High overhydration risk; possible emergency |
Consensus in sports medicine supports “drink to thirst,” commonly ~0.4–0.8 L/hour for endurance efforts, with higher amounts only for very heavy sweaters in extreme heat.
Electrolyte Balance: Why Water Alone Isn’t Enough
Electrolytes—sodium, potassium, chloride, magnesium—support nerve signaling and muscle contraction. Moreover, in heat or long exercise, you lose water and sodium together; replacing only water can dilute remaining electrolytes.
Practical Sodium Targets (Start Here)
- To start: aim for ~200–300 mg sodium per hour for extended exercise; then adjust to your sweat rate and saltiness.
- For context: many sports drinks supply ~460–690 mg sodium per liter (20–30 mEq/L). If you drink 0.5–1.0 L/hour, that’s roughly ~230–690 mg sodium/hour.
- If you’re a heavy/salty sweater: you may need higher amounts in hot, long efforts—therefore, confirm with sweat testing and performance feedback.
- Caveat: electrolytes help replace losses but do not prevent hyponatremia if you overdrink; consequently, prioritize pacing fluids and monitoring weight.
Quick Sodium Guide (Simple & Practical)
Teaspoon → mg sodium: 1 tsp ≈ 2,300 mg • ½ tsp ≈ 1,150 mg • ¼ tsp ≈ 575 mg • ⅛ tsp ≈ 290 mg • a pinch (1/16 tsp) ≈ 145 mg
- DIY 1-liter bottle: Water + ⅛ tsp table salt (≈ 290 mg sodium per liter). Sip ~0.7 L/hour → ~200 mg/hour or ~1.0 L/hour → ~290 mg/hour.
- Use the label: Sodium per hour = (mg per serving ÷ serving volume) × how much you drink per hour. Example: drink has 500 mg/L and you sip 0.5 L/hour → about 250 mg/hour.
- Quick top-up: If your drink is low sodium, add a pinch (~145 mg) to your hourly bottle. Two pinches ≈ ~290 mg.
Sanity checks: avoid body-mass gain during long sessions. If you cramp and have very salty sweat, nudge sodium up slowly.
Health note: If you have high blood pressure, kidney/heart conditions, or a doctor-prescribed low-sodium diet, don’t add salt without medical guidance.
Hydration Assessment: Your Body’s Built-in Gauge
As a quick screen, use urine color alongside thirst and performance.
- Clear: possible overhydration
- Pale yellow: typical/ideal
- Dark yellow: likely need more fluids
- Dark brown: seek medical attention promptly
Validated urine color scales are widely used by athletic programs; additionally, they are easy to apply at home.
Calculate Your Personal Sweat Rate (NASM-style)
1) Weigh yourself (minimal clothing) BEFORE exercise
2) Exercise for ~60 minutes; note all fluids you drink
3) If you urinate during the test, estimate that volume (optional)
4) Towel dry and weigh AFTER exercise (same scale, same clothing)
5) Sweat rate (L/h) = [(Pre-weight − Post-weight) in kg + Fluids (L) − Urine (L)] ÷ Exercise time (h)
6) Rehydrate ~150% of weight lost over the next 2–4 hoursRepeat in different conditions (heat, humidity, intensity) to build your personal ranges. Note: 1 kg mass change ≈ 1 liter of fluid.
Safe Hydration Alternatives
Instead of chasing a fixed gallon goal, try the practical options below. Consequently, most people find pacing easier and safer.
- 16–24 oz bottles: easier pacing & tracking
- Electrolyte timing: add sodium for >60–90 min or heavy sweat
- Food-first: fruit, yogurt, broth contribute fluids & electrolytes
- Room-temp water: often easier to drink than ice-cold
- Mindful sipping: steady intake vs. chugging

Evidence-Based Hydration Guidelines for Daily Life
Daily Schedule
- Morning: 16–20 oz over the first 2 hours
- Pre-exercise: 8–16 oz ~30 minutes before
- During exercise: 6–8 oz every 15–20 minutes (adjust for thirst, heat, sweat rate)
- After exercise: 16–24 oz over 1–2 hours; include salty food or an electrolyte drink after longer sessions
- Evening: 8–12 oz; stop ~2 hours before bed
Daily Totals
In general, daily fluid amounts are ~2.7 L/day (women) and ~3.7 L/day (men) from beverages + food. Nevertheless, about 20–30% typically comes from food; hotter climates and higher activity raise needs.
Medical Emergency: When Water Becomes Dangerous
Recognize these patterns early; if symptoms escalate, act immediately.
Severe Dehydration
- Little to no urination for many hours
- Extreme thirst, dry mouth, dizziness
- Rapid heartbeat; sunken eyes/cheeks
Water Intoxication / Hyponatremia
- Severe headache unrelieved by OTC meds
- Nausea/vomiting, confusion, seizures
- Muscle weakness/cramping, loss of consciousness
Heat-Related Illness
- Core temp ≥ 103°F (39.4°C)
- Altered mental state/behavior
- Hot, dry skin or profuse sweating; rapid, strong pulse
These can be life-threatening. Therefore, call 911 or local emergency services immediately.
Professional Hydration Guide (NASM-Style Upgrades)
Use this step-by-step guide to individualize hydration for training, events, and hot conditions. Adjust based on your own responses and the guidance of qualified professionals.
1) NASM Sweat Rate Testing Protocol
Follow the detailed steps in Calculate Your Personal Sweat Rate, then log results across different conditions to build low/typical/high ranges.
- Test in cool, moderate, and hot weather; repeat for easy vs. hard sessions.
- Use consistent scales/clothing; 1 kg mass change ≈ 1 L fluid.
- Build your working range (e.g., 0.45–0.70 L/h typical; 0.65–0.85 L/h hot).
2) Pre-Exercise Hydration Assessment
- 2–4 hours pre: ~5–7 mL/kg body mass (add sodium if you’re a heavy/salty sweater or first-morning urine is dark).
- 10–20 minutes pre (optional): If urine remains dark and no contraindications, add 3–5 mL/kg.
- Morning baseline: Track first-morning urine color; aim for pale yellow on training days.
- Multi-day events: Track morning body weight. A drop of >2% from baseline signals under-recovery → increase fluids/electrolytes and nutrition.
3) Environmental Condition Protocols
Heat Index (HI) Guidance
| HI Category | Typical Fluid Pace | Sodium (start point) | Notes |
|---|---|---|---|
| Low (< 80°F / 27°C) | 0.4–0.6 L/h | 200–300 mg/h | Standard plan |
| Moderate (80–90°F / 27–32°C) | 0.5–0.7 L/h | 300–500 mg/h | Plan shade/cooling breaks |
| High (90–104°F / 32–40°C) | 0.6–0.8 L/h | 400–600 mg/h | Increase cooling frequency |
| Very High (> 104°F / 40°C) | Shorten/postpone | As needed | Aggressive cooling; consider cancellation |
Humidity
High humidity / dew point > 65°F (18°C) slows evaporation → expect higher sweat rates. Nudge fluids by ~+0.1–0.2 L/h; prioritize cooling strategies (ice towels, cold fluids, shade).
Altitude
Above ~1,500 m, respiratory water loss rises. Add ~0.5–1.0 L/day overall; keep sodium adequate; monitor morning weight/urine color.
Acclimatization
Allow 7–14 days. Early: shorter/easier sessions, more cooling, slightly higher sodium. Progress duration/intensity gradually.
4) More Precise Electrolyte Timing
- < 60 minutes: Water usually sufficient.
- 60–90 minutes (high-intensity): Consider electrolytes; start ~200–300 mg sodium/hour.
- > 90 minutes: Electrolytes recommended; many do well at ~200–300 mg/h, more if very salty sweater.
- Typical sports drink: ~460–690 mg sodium/L (20–30 mEq/L). If you drink 0.5–1.0 L/h, that’s ≈ 230–690 mg/h.
- Caution: Electrolytes don’t prevent hyponatremia if you overdrink. Pace to thirst and avoid weight gain during long events.
5) Hydration Periodization for Athletes
- Base phase: Build daily habits; test sweat rate; practice “drink to thirst” around 0.4–0.8 L/h.
- Competition: Script pre-event fluids (5–7 mL/kg 2–4 h pre; optional 3–5 mL/kg top-off). During: avoid body-mass gain; plan access/cooling.
- Recovery: Replace ~125–150% of mass lost (1.25–1.5 L per kg) with sodium; pair with carbs/protein.
- Multi-day: Morning weigh-ins, urine color, and symptom checks to adapt daily plan.
- Load monitoring: Track RPE, resting HR/HRV, sleep, and mood; adjust fluids/electrolytes with training stress.
6) Practical Assessment Tools
- Thirst scale (1–9): 1–2 well-hydrated; 3–5 normal; 6–7 thirsty; 8–9 very thirsty → drink and cool.
- Performance signs: Rising HR at given pace/power, unusual RPE, or cramping → review fluids/electrolytes.
- Recovery checks: Morning weight (±2%), urine color, sleep quality, mood.
- Field signs: Lightheaded on standing, persistent headache, nausea → pause, cool, reassess hydration plan.
Quick mass check: Post-session body mass up = overdrank; down > 2% = underhydrated.
7) Scope of Practice Language
- These are general guidelines; individual needs vary.
- Work with qualified professionals (sports dietitian, physician) for personalized plans.
- Monitor your responses and adjust with changes in heat, altitude, training, or health.
- Education only — not medical advice. Seek medical guidance for kidney/cardiac/endocrine issues, pregnancy, or pediatric needs.
8) Evidence-Based Supplement Integration
- When water isn’t enough: > 60–90 min, hot/humid, high sweat rates, or known salty sweaters.
- Options: Commercial sports drinks/tablets; food-first choices like broths, salted pretzels, pickles, tomato juice.
- Timing: Small, frequent sips during; include sodium in post-exercise rehydration to improve retention.
- DIY 1 L mix: Water + ¼ tsp table salt (~590 mg sodium) + 1–2 Tbsp sugar or honey + citrus. Adjust to taste and sweat rate.
Priority Order for Implementation
High: #1 Sweat rate testing, #4 Electrolyte timing, #7 Scope of practice
Medium: #2 Pre-exercise assessment, #6 Assessment tools, #3 Environmental protocols
Lower: #5 Periodization, #8 Supplement integration
Scientific References and Clinical Research
- Clinical Journal of Sport Medicine: Exercise-Associated Hyponatremia Consensus (2017)
- New England Journal of Medicine: Hyponatremia among Boston Marathon Runners
- Medicine & Science in Sports & Exercise: Exercise & Fluid Replacement Position Stand
- International Journal of Sport Nutrition & Exercise Metabolism: Overhydration Research
- Clinical Journal of the American Society of Nephrology: Kidney Water Excretion Physiology
- British Journal of Sports Medicine: Personalized Hydration Strategies
- Journal of Athletic Training: Electrolyte Replacement Research
- Journal of Sports Medicine & Physical Fitness: Urine Color Assessment
- Nutrients: Daily Fluid Intake Requirements & Clinical Applications
- American Journal of Emergency Medicine: Recognition & Treatment of Water Intoxication
- Cyberpsychology: Risks of Viral Health Challenges
- Mayo Clinic: Hyponatremia
- CDC: Water & Healthier Drinks
- AAP: Sports & Energy Drinks for Children & Adolescents
- ACSM: Exercise & Fluid Replacement (PDF)
Additional Research Resources
- International Journal of Environmental Research & Public Health: Water Container Safety
- Case Reports in Emergency Medicine: Social Media Challenge Hospitalizations
- MSSE (2016): Fluid Balance & Dehydration in the Athlete
- Pediatrics (AAP): Youth Health Guidance
- Geriatric Medicine Research: Age-Related Hydration Changes
Frequently Asked Questions
Is drinking a gallon a day safe?
Context matters. Rapid chugging for hours can cause hyponatremia. Pace ~0.4–0.8 L/hour and avoid weight gain.
How much can kidneys process per hour?
In ideal conditions ~0.8–1.0 L/hour. Heat, stress, nausea, or low solute lower this practical limit.
Signs of overhydration?
Headache, nausea, bloating, confusion. Severe: seizures or fainting—seek emergency care.
What’s a safe plan during exercise?
Start ~0.4–0.8 L/hour; consider 200–300 mg sodium/hour for longer or hot efforts. Adjust to thirst and sweat rate.
Can electrolytes prevent hyponatremia?
No. They replace losses but don’t prevent dilution if you overdrink. Pace fluids first.
Is clear urine all day good?
Not always. It can indicate overhydration. Aim for pale yellow most of the day.
How fast is too fast to drink?
Rapid chugging for hours is risky. Smaller, steady sips matched to thirst are safer.
Heat illness vs. hyponatremia?
They overlap (headache, nausea). Heavy water intake + confusion suggests hyponatremia. If unsure, seek care.
Want more? See the full Q&A in our guide above and download the
Smart Hydration Tracker (PDF).
